Our top priority is the health of your eyes. We want to keep your eyes healthy through regular eye health evaluations, communication and education. This page lists a few of the most common eye diseases. Select from the following list of topics or scroll to learn about the causes, symptoms, and treatments for:
| Cataract | Conjunctivitis | Diabetic Retinopathy |
| Dry Eye Syndrome | Glaucoma | Macular Degeneration |
| Retinal Detachment | example |
Blepharitis
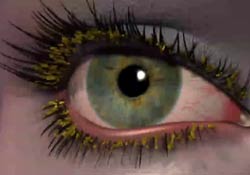 There are three types of anterior blepharitis. Seborrheic blepharitis is often part of an overall skin condition called seborrhea, which may also affect the scalp, chest, back and the area behind the ears. The second form of blepharitis – staphylococcal blepharitis – is a more severe condition, caused by bacteria. The third form of blepharitis is Demodex blepharitis caused by Demodex mites, which are very tiny parasites that live at the base of the eyelash. Unfortunately as we get older they are more common.
There are three types of anterior blepharitis. Seborrheic blepharitis is often part of an overall skin condition called seborrhea, which may also affect the scalp, chest, back and the area behind the ears. The second form of blepharitis – staphylococcal blepharitis – is a more severe condition, caused by bacteria. The third form of blepharitis is Demodex blepharitis caused by Demodex mites, which are very tiny parasites that live at the base of the eyelash. Unfortunately as we get older they are more common.
Causes
Hormones, nutrition, general physical condition, and even stress may contribute to seborrheic blepharitis. Build-ups of naturally occurring bacteria contribute to staph blepharitis.
Symptoms
Seborrheic blepharitis results in redness of the eyelids, flaking and scaling of eyelashes, and greasy, waxy scales. Staph blepharitis presents with debris, collarettes and sometimes discharge on the lid and can cause small ulcers, loss of eyelashes, eyelid redness, thickening, scarring and even red eye. Demodex blepharitis presents as a sleeve around the base of the lashes.
Treatment
Careful cleaning of the eyelids can reduce seborrheic blepharitis as well as use of steroid cream or ointment. Application of hot packs to the eyes for 20 minutes a day can also help. Staph blepharitis may require topical antibiotic or antibiotic/anti-inflammatory combination drops or ointments. Treatment for Demodex may include tea tree oil shampoo or bland ointments to suffocate the mites and eggs.
Cataracts
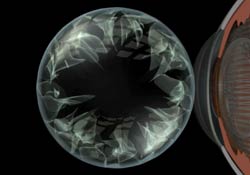 A cataract is cloudiness (opacification) that develops in the lens of the eye from aging, trauma, medication or disease. It can also form during fetal development and be present at birth. The lens is made mostly of water and protein that is arranged to allow light through undisturbed but as the lens becomes cloudy from the cataract, light is blocked and scattered reducing vision.
A cataract is cloudiness (opacification) that develops in the lens of the eye from aging, trauma, medication or disease. It can also form during fetal development and be present at birth. The lens is made mostly of water and protein that is arranged to allow light through undisturbed but as the lens becomes cloudy from the cataract, light is blocked and scattered reducing vision.
Symptoms
A person with cataracts may encounter faded colors, problems with light (such as halos, or headlights that seem too bright), poor night vision, double vision, or multiple vision.
Treatment
We can diagnose the presence and density of cataracts during a thorough eye exam through dilated pupils. Treatment is surgical removal of the cloudy lens and replacement with a clear intraocular lens.
Conjunctivitis
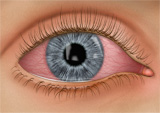 Conjunctivitis, commonly called pink eye, is an infection or inflammation of the conjunctiva of the eye causing redness and discharge as well as puffiness or swelling of the lids. Discharge will vary (watery, pus, or stringy/ropey) based on the nature of the infection/inflammation (viral, bacterial, allergic).
Conjunctivitis, commonly called pink eye, is an infection or inflammation of the conjunctiva of the eye causing redness and discharge as well as puffiness or swelling of the lids. Discharge will vary (watery, pus, or stringy/ropey) based on the nature of the infection/inflammation (viral, bacterial, allergic).
Causes
Pink eye is most commonly caused by a viral infection but may also be caused by a bacterial infection or an allergic response. Viral and bacterial conjunctivitis are very contagious.
Prevention and Treatment
To avoid spreading conjunctivitis, wash your hands often, do not touch the infected area with your hands, do not share wash cloths or towels and avoid using makeup which may become contaminated. A child with pink eye should be kept from school for a few days. Sometimes the eye doctor will need to prescribe antibiotic eye drops and ointments to clear up conjunctivitis.
Diabetic Retinopathy
Diabetes damages blood vessels compromising their integrity. This leads to blockage and or leakage of blood into the retina reducing normal blood flow. If blood flow is significantly compromised, new blood vessels may form (neovascularization) to replace the damaged vessels to try to restore normal blood flow to the retina. Unfortunately, the new blood vessels are abnormal and fragile and can rupture causing more bleeding, blurred vision or eventual blindness. The poorer your diabetic control the more likely retinopathy will develop, which is why it is so important to maintain the utmost compliance with your medications, diet and exercise regimen.
Symptoms of diabetic retinopathy:
There may be no symptoms in the early stages of the disease, which is why it’s important for diabetics to have an annual exam with dilation to monitor the retina. However, if fluid leaks into the macula, which is the area where best vision (20/20) occurs, this will cause swelling of the tissue and blurry vision. Other symptoms include fluctuating vision, empty areas in your field of vision and difficulty with color vision.
Risk Factors and Treatment
If you have diabetes, it’s critical to control your blood sugar level. This will reduce your risk of getting diabetic retinopathy. If you are experiencing some of the symptoms listed above, call us for an appointment. If diagnosed in time, these complications can be treated with medications, laser or surgery (vitrectomy) to try to control and reduce the damage from the retinopathy. Diabetics are also more prone to developing cataracts at an earlier age than the average person and are at higher risk to develop glaucoma.
Dry Eye Syndrome
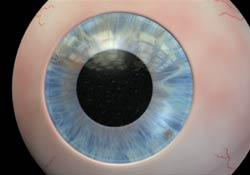 Dry eye syndrome affects almost 10 million Americans and occurs as we age, usually starting in our 40s. Dry eye syndrome is caused by a lack of tears or poor quality tears. Tears are critical for lubricating the surface of the eye and are composed of three layers: the outer oily layer, the middle aqueous (water) layer and the inner mucous layer next to the cornea. If any of the tear layers become compromised from lack of mucous, water or oil, the eye becomes uncomfortable.
Dry eye syndrome affects almost 10 million Americans and occurs as we age, usually starting in our 40s. Dry eye syndrome is caused by a lack of tears or poor quality tears. Tears are critical for lubricating the surface of the eye and are composed of three layers: the outer oily layer, the middle aqueous (water) layer and the inner mucous layer next to the cornea. If any of the tear layers become compromised from lack of mucous, water or oil, the eye becomes uncomfortable.
Symptoms
Dry eye syndrome leads to a number of symptoms including irritation, burning, gritty sandy feeling, pain or soreness, reflex tearing, redness, occasional itching, discomfort or blurring in windy conditions, blurred vision that improves with blinking and discomfort after long periods of watching television, using a computer or reading.
Treatment
Dry eyes can be treated with the use of over-the-counter artificial tears/gels/ointments, prescription eye drops, oral medication, punctal plugs, nutritional supplements and expression of plugged glands. Some artificial tear brands may work better than others depending on the cause of your dry eyes.
Risk Factors
There are many factors that can contribute to dry eyes such as dry, hot, or windy climate; air pollution, cigarette smoke, high altitudes and air-conditioning or heaters. Contact lens wearers may not have enough tears to keep the lenses hydrated during wear causing dryness. You may also be more at risk if you have a thyroid condition, a vitamin-A deficiency, arthritis, lupus, Parkinson’s, Sjogren’s, rosacea, diabetes, sarcoidosis, sleep disorders, herpes zoster or if you are a woman going through menopause. Medications can cause dryness such as anti-depressants, antihistamines, decongestants, diuretics, beta blockers, oral contraceptives, hormone replacement therapy, and ulcer or incontinence medication.
Glaucoma
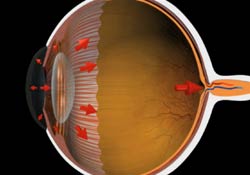 Glaucoma is a common eye disorder affecting millions of Americans. It is caused by too much pressure inside the eye. Fluid called aqueous is constantly being produced inside the eye and constantly flowing out of the angle of the eye. If aqueous is prevented from flowing out, the intraocular pressure builds and damages the optic nerve causing gradual reduction of your visual field and eventual blindness.
Glaucoma is a common eye disorder affecting millions of Americans. It is caused by too much pressure inside the eye. Fluid called aqueous is constantly being produced inside the eye and constantly flowing out of the angle of the eye. If aqueous is prevented from flowing out, the intraocular pressure builds and damages the optic nerve causing gradual reduction of your visual field and eventual blindness.
Symptoms
It’s hard to notice symptoms because of the gradual progression of the disease. Those suffering from open-angle glaucoma experience tunnel vision over time where their field of vision slowly declines. Narrow-angle glaucoma, which is not as common as open angle, is caused by internal eye structures blocking outflow of aqueous. Patients can experience a narrow angle attack that carries symptoms of sharp pain in the eyes, blurred vision, mid-dilated pupils and even nausea or vomiting. Immediate medical attention is needed to stop the attack.
Risk Factors
Heredity seems to be a risk factor. Also, you may be at greater risk if you are over 45, of African descent, near-sighted or diabetic. Finally, if you have used steroids or for a long period of time or if you have suffered an eye injury in the past, you have a greater chance of developing glaucoma.
Treatment
Treatment of glaucoma entails the use of medicine (eye drops), laser treatment and surgery.
Keratoconus
Keratoconus is a degenerative disorder of the cornea usually developing during the teenage years. Keratoconus causes thinning of the corneal tissue which compromises its structural integrity. The cornea becomes weakened and bulges forward leading to distortion of its normal shape by creating high degrees of irregular astigmatism, nearsightedness and very blurry vision. Glasses may work well initially, however, as the disorder progresses, toric soft lenses, custom soft Keratoconus lenses, rigid gas permeable corneal contact lenses or Scleral gas permeable contact lenses will become the better options for clear functional vision. Corneal Cross-Linking (FDA approval pending) and Intrastromal Corneal Ring Segments (Intacs) have been used to try to stabilize the condition. Worse case scenario occurs when the cornea becomes so physiologically and functionally degraded that a Corneal Transplant/Graft is necessary. After Corneal Transplant/Graft, individuals may find that a Scleral contact lens may still be required to provide clear vision. At Nevada Eye Care Optometry we specialize in prescribing these lenses.
Macular Degeneration
Macular degeneration is a disease which affects a small area of the retina known as the macula. The macula is a highly pigmented specialized area of the retina about 5mm in diameter that allows us to see fine detail of whatever is directly in front of us. Macular degeneration occurs when the macula begins to break down and deteriorate.
“Wet” vs. “Dry”
Most often, macular degeneration is accompanied by formation of yellow deposits, called “drusen,” under the macula, which compromise the health of the macula. This is called “dry” macular degeneration. In some cases, abnormal blood vessels (neovascularization) develop under the macula and leak fluid. This is called “wet” macular degeneration.
Causes
A number of uncontrollable factors contribute to macular degeneration, including heredity, age, sex, eye color, farsightedness, and race. Risk factors you can control include smoking, high blood pressure, exposure to harmful sunlight and diet. Considerable research is being conducted into causes of the disease.
Symptoms
It is difficult to detect dry macular degeneration in its early stages. The most common symptoms, when detected, include a spot of blurry, dark or distorted vision in your central field of vision not correctable with glasses. Wet macular degeneration progresses much faster than the dry variety. Both forms of macular degeneration can lead to loss of central vision such that there is a blind spot in the center of your visual field.
Treatment
Currently, there is no cure for macular degeneration, but nutritional supplements and medical treatment are available to try to slow progression. A tremendous amount of research is being conducted for treatment of macular degeneration because as we live longer, more and more people develop the disease.
Retinal Detachment
The retina is the light sensitive neurological tissue lining the inside of the back of the eye. It translates light rays into electrical signals for transmittance along the optic nerve to the occipital lobe of the brain (visual cortex). When the retina separates (falls off or tears) from the back of the eye, it is known as a retinal detachment. It is a serious condition which can cause permanent tissue damage and vision loss if not treated in a timely manner.
Symptoms
A retinal detachment often causes sudden defects in your vision. It may just cause a blind spot too small to notice or it may cause a noticeable shadow which obscures your vision. An increase in “floaters,” which look like small particles, specks or fine threads, may also be noticed. Finally, flashes of light are associated with retinal detachment because the mechanical action of the detachment sets off photoreceptors in the retina causing the flash of light.
Risk Factors
Eye injuries, tumors and cataract surgery can cause retinal detachment. Near-sighted individuals and the elderly are at greater risk for spontaneous detachment. Also, significant diabetic retinopathy can lead to retinal detachment.
Treatment
Retinal detachment requires surgical treatment in a timely manner because of its urgency.





